Biting Insects
 Most mandibulate insects are not strong enough to pierce human skin with their mouthparts. Their bite is usually little more than a pinch, serving primarily as a defensive behavior (e.g. ground beetles and ants). Even fire ants (Solenopsis spp.), whose painful “bite” is well known, lack the ability to penetrate skin. In fact, their “bite” is actually caused by a sting at the other end of the body!
Most mandibulate insects are not strong enough to pierce human skin with their mouthparts. Their bite is usually little more than a pinch, serving primarily as a defensive behavior (e.g. ground beetles and ants). Even fire ants (Solenopsis spp.), whose painful “bite” is well known, lack the ability to penetrate skin. In fact, their “bite” is actually caused by a sting at the other end of the body!
All of the arthropods that can pierce human skin have mouthparts that are especially adapted for piercing, cutting, or burrowing. These include:
- Diptera (mosquitoes, black flies, horse flies, deer flies, stable flies, sand flies, and various biting midges)
- Hemiptera, (bed bugs, assassin bugs, water bugs)
- Thysanoptera (thrips)
- Psocodea (sucking lice)
- Siphonaptera (fleas)
- the class Arachnida (spiders, mites, and ticks).
 Most of these arthropods are hematophagous (they feed on blood). Their mouthparts are designed either to cut the skin and induce bleeding (horse flies and stable flies) or to pierce far enough under the skin to reach capillary blood (mosquitoes, bugs, fleas, etc.). Salivary enzymes and other compounds, such as anti-coagulants, anesthetics, and vasodilators also may be injected by the mouthparts during feeding. The localized reaction to an insect bite (pain, swelling, redness, etc.) is usually a physiological (inflammatory) response to these injected compounds.
Most of these arthropods are hematophagous (they feed on blood). Their mouthparts are designed either to cut the skin and induce bleeding (horse flies and stable flies) or to pierce far enough under the skin to reach capillary blood (mosquitoes, bugs, fleas, etc.). Salivary enzymes and other compounds, such as anti-coagulants, anesthetics, and vasodilators also may be injected by the mouthparts during feeding. The localized reaction to an insect bite (pain, swelling, redness, etc.) is usually a physiological (inflammatory) response to these injected compounds.
 Although the amount of blood taken by each insect may be quite small, the cumulative effects of blood feeding by large populations of hematophagous insects can be life-threatening. In the summertime, small herds of reindeer living above the arctic circle have died from desanguination (massive loss of blood) caused by hoards of mosquitoes and black flies.
Although the amount of blood taken by each insect may be quite small, the cumulative effects of blood feeding by large populations of hematophagous insects can be life-threatening. In the summertime, small herds of reindeer living above the arctic circle have died from desanguination (massive loss of blood) caused by hoards of mosquitoes and black flies.
 Some arachnids (e.g. spiders) and most water bugs (Notonectidae, Belostomatidae, and Gerridae, for example) bite only defensively. Their strong, piercing mouthparts can inject toxins or digestive enzymes that may cause pain and localized swelling. In North America, the black widow spider (Latrodectus mactans), the brown recluse spider (Loxosceles reclusa), and two species of scorpions (Centruroides sculpturatus and C. gertschi) are the only arthropods with a venom that is toxic enough to cause serious illness or death.
Some arachnids (e.g. spiders) and most water bugs (Notonectidae, Belostomatidae, and Gerridae, for example) bite only defensively. Their strong, piercing mouthparts can inject toxins or digestive enzymes that may cause pain and localized swelling. In North America, the black widow spider (Latrodectus mactans), the brown recluse spider (Loxosceles reclusa), and two species of scorpions (Centruroides sculpturatus and C. gertschi) are the only arthropods with a venom that is toxic enough to cause serious illness or death.
Itch mites, mange mites, and harvest mites (chiggers or redbugs), burrow into the skin of humans and other animals where they feed on body fluids and tissues. These infestations (variously known as acariasis, mange, or scabies) cause redness, itching, and flaking of the skin. The itch mite, Sarcoptes scabiei hominis, causes a severe, itching rash in humans; other subspecies of the same mite infest dogs, swine, cattle, and sheep. Infestations of various mites can become a severe economic problem in commercial poultry and swine production. The northern fowl mite, Ornithonyssus sylviarum, is a fast breeding pest that lives around the neck, vent, and tail of chickens. Under ideal conditions, this species completes its life cycle in less than seven days. Population growth is explosive, and often difficult to control.
Thrips have rasping/sucking mouthparts capable of abrading the skin and causing irritation. These insects are primarily herbivores, but they may be quite annoying to people who work near infested plants. Occasional reports of predatory thrips that suck blood are unsubstantiated.
Stinging Insects
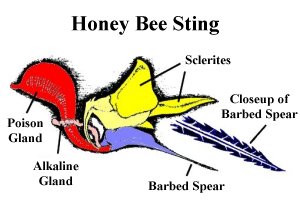 Ants, wasps, bees, and scorpions are the only arthropods that have a true stinger. Some predatory and parasitic insects sting to kill or immobilize their prey, whereas most other species sting only as a defensive behavior to kill or drive away potential predators. In all of the stinging (aculeate) hymenoptera, the stinger is modified from structures of the ovipositor. The shaft of the stinger is hollow, occasionally barbed, and connected internally to a venom gland that produces a complex mixture of compounds that may destroy cells (hemolytic and proteolytic enzymes), increase blood flow (hemorrhagic enzymes), break down intercellular connective tissue (hyaluronidase), and cause neurotoxic or other pharmacologic effects on nerve cells.
Ants, wasps, bees, and scorpions are the only arthropods that have a true stinger. Some predatory and parasitic insects sting to kill or immobilize their prey, whereas most other species sting only as a defensive behavior to kill or drive away potential predators. In all of the stinging (aculeate) hymenoptera, the stinger is modified from structures of the ovipositor. The shaft of the stinger is hollow, occasionally barbed, and connected internally to a venom gland that produces a complex mixture of compounds that may destroy cells (hemolytic and proteolytic enzymes), increase blood flow (hemorrhagic enzymes), break down intercellular connective tissue (hyaluronidase), and cause neurotoxic or other pharmacologic effects on nerve cells.
 Arthropod venom is rapid-acting and frequently associated with considerable pain. Most people experience an intense local reaction that subsides after several hours and heals within a few days. But for other people (estimates range from 2-5% of the U.S. population) a single sting may elicit anaphylactic shock, a life-threatening allergic reaction caused by hypersensitivity to insect protein or any other venom component. Anaphylaxis is characterized by rapid loss of blood pressure, fainting, and respiratory difficulty. If the patient does not receive prompt medical attention, unconsciousness and death may occur within minutes. Emergency treatment of anaphylactic shock usually consists of deep subcutaneous or intramuscular injections of a cardiac stimulant (such as norepinephrine) in an effort to counteract the physiological reaction, increase heart rate, and stabilize blood pressure. Emergency bee sting kits, containing auto-injectable norepinephrine, are available by prescription to patients with known sensitivity to insect stings. In the United States, about 20 deaths per year are attributed to stinging insects — in nearly every case death results from anaphylactic shock, not the sting itself.
Arthropod venom is rapid-acting and frequently associated with considerable pain. Most people experience an intense local reaction that subsides after several hours and heals within a few days. But for other people (estimates range from 2-5% of the U.S. population) a single sting may elicit anaphylactic shock, a life-threatening allergic reaction caused by hypersensitivity to insect protein or any other venom component. Anaphylaxis is characterized by rapid loss of blood pressure, fainting, and respiratory difficulty. If the patient does not receive prompt medical attention, unconsciousness and death may occur within minutes. Emergency treatment of anaphylactic shock usually consists of deep subcutaneous or intramuscular injections of a cardiac stimulant (such as norepinephrine) in an effort to counteract the physiological reaction, increase heart rate, and stabilize blood pressure. Emergency bee sting kits, containing auto-injectable norepinephrine, are available by prescription to patients with known sensitivity to insect stings. In the United States, about 20 deaths per year are attributed to stinging insects — in nearly every case death results from anaphylactic shock, not the sting itself.
 The larvae of certain flannel moths (Megalopygidae) and slug caterpillars (Limacodidae) do not have a stinger, but they also inflict a sharp, stinging pain upon contact.
The larvae of certain flannel moths (Megalopygidae) and slug caterpillars (Limacodidae) do not have a stinger, but they also inflict a sharp, stinging pain upon contact.
These insects have specialized urticating hairs that inject a painful chemical when touched. The sensation, like that of a stinging nettle, is an intense localized pain that gradually fades after several hours. More about
stinging caterpillars Saddleback caterpillars (Sibine stimulea) are probably the most conspicuous of the stinging caterpillars. They feed on a variety of trees and shrubs, including cherry, plum, elm, and poplar.
Irritants and Allergens
 Skin and eye irritation, respiratory inflammation, and various types of chronic allergies may also be caused by insects and related arthropods. An allergic reaction can be induced by nearly any component of an insect’s body, but hairs, scales, exuviae, and fecal products are the most common culprits. Allergies to household dust, for example, can often be traced to dander from fleas (Siphonaptera), cockroaches (Blattodea), or house dust mites (Dermatophagoides spp.). Larvae of the browntail moth (Euproctis chrysorrhoea) have hairs that cause an irritating rash on the skin of many people.
Skin and eye irritation, respiratory inflammation, and various types of chronic allergies may also be caused by insects and related arthropods. An allergic reaction can be induced by nearly any component of an insect’s body, but hairs, scales, exuviae, and fecal products are the most common culprits. Allergies to household dust, for example, can often be traced to dander from fleas (Siphonaptera), cockroaches (Blattodea), or house dust mites (Dermatophagoides spp.). Larvae of the browntail moth (Euproctis chrysorrhoea) have hairs that cause an irritating rash on the skin of many people.
Human exposure to sensitizing antigens usually occurs in one of four ways:
- inhalation of airborne particles
- ingestion with foods
- dermal contact, or
- unintentional injection (as by rubbing the eyes)
Immunological responses of the human body vary, but sneezing, watery eyes, a runny nose, or skin rashes are common manifestations. Chronic asthma, allergic rhinitis, and eczema are frequently aggravated by exposure to arthropod antigens.
The prognosis for treatment of “arboallergies” is not very promising. One option, immunotherapy, involves successive exposures to increasing concentrations of the offending allergen in an effort to desensitize the immune system. This approach may provide some relief for some patients, but the only “sure cure” is complete avoidance of exposure to the allergens.
Myiasis
 Of all the arthropods, only the larvae of certain flies (Diptera) are adapted to invade and consume the tissues of a vertebrate host. An infestation by any of these flies is known as myiasis. In North America, this type of parasitism is most common among domestic animals (particularly sheep, cattle, and horses), but it can also be a problem among the poor and elderly of the human population where it is usually associated with neglect and unsanitary conditions.
Of all the arthropods, only the larvae of certain flies (Diptera) are adapted to invade and consume the tissues of a vertebrate host. An infestation by any of these flies is known as myiasis. In North America, this type of parasitism is most common among domestic animals (particularly sheep, cattle, and horses), but it can also be a problem among the poor and elderly of the human population where it is usually associated with neglect and unsanitary conditions.
Some of these flies breed in carrion or manure; others live in spoiled food. Eggs or larvae may be ingested and survive in the vertebrate’s intestinal tract, or larvae may crawl into the bowel through the anus. The screwworm fly (Cochliomyia hominivorax) lays its eggs in open, festering wounds. Larvae feed on these injured tissues and prevent healing. Screwworms are endemic to Mexico and the southwestern United States where they are a major pest of sheep and cattle. A sterile-male release program (see Chapt. 19) has eradicated screwworm populations from Texas and New Mexico, but ranchers in southern Mexico still suffer heavy losses from these flies.
The family Oestridae includes warble flies, cattle grubs, and bot flies whose larvae also parasitize domestic animals. Cattle grubs (Hypoderma bovis and H. lineatum) lay their eggs on the legs of cattle. After hatching, larvae burrow through the skin and migrate upward, first to the digestive system and eventually to the back where they produce swellings known as “warbles”. Full grown larvae cut their way out of the warble leaving a hole that decreases the hide’s value when it is tanned for leather. The sheep bot fly (Oestrus ovis) produces live young and deposits them in the nostrils of sheep. These larvae migrate into the sinus cavities where they complete development. Large fly populations can weaken or kill the sheep.
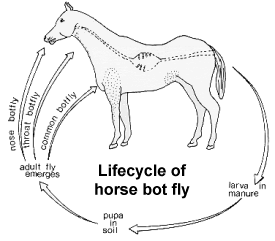 Larvae of flies in the family Gastrophilidae (the horse bot flies) are internal parasites of horses and mules. Most species lay their eggs around the animal’s nose or mouth. After hatching, the larvae burrow or crawl into the horse’s mouth and eventually move down the digestive tract, attaching themselves to the walls of the stomach, duodenum, or rectum. The horse bot fly (Gasterophilus intestinalis) lays its eggs on the legs, flanks, or shoulders of the horse. These eggs hatch immediately when they are licked and ingested by the horse. The presence of bots (fly larvae) in the animal’s digestive system often causes malnutrition, ulceration of the digestive tract, and even complete blockage of the intestine. Mature larvae leave their vertebrate host by passing out as excrement. They pupate in the soil and emerge as adults several weeks later.
Larvae of flies in the family Gastrophilidae (the horse bot flies) are internal parasites of horses and mules. Most species lay their eggs around the animal’s nose or mouth. After hatching, the larvae burrow or crawl into the horse’s mouth and eventually move down the digestive tract, attaching themselves to the walls of the stomach, duodenum, or rectum. The horse bot fly (Gasterophilus intestinalis) lays its eggs on the legs, flanks, or shoulders of the horse. These eggs hatch immediately when they are licked and ingested by the horse. The presence of bots (fly larvae) in the animal’s digestive system often causes malnutrition, ulceration of the digestive tract, and even complete blockage of the intestine. Mature larvae leave their vertebrate host by passing out as excrement. They pupate in the soil and emerge as adults several weeks later.
Transmission of Diseases
 Infectious agents that cause illness or disease in other living organisms are known as pathogens. These agents may include a wide variety of microorganisms (e.g. mycoplasmas, bacteria, protozoa, spirochetes, and rickettsias) as well as fungi, helminths (roundworms and flatworms), and viruses. A host is any living organism that is infected by a pathogen, regardless of whether or not symptoms of the disease are present. Some hosts die quickly, others may kill or inactivate the pathogen, and still others may retain the pathogen in a condition of readiness to infect other hosts. Whenever a host serves as a source of new infections for other hosts (of the same or different species) it is known as a reservoir. Since pathogens do not have legs or wings, they are often “carried” from one host to another by vectors. Insects and related arthropods are among the most important vectors of pathogens. The term zoonosis (or zoonotic disease) refers to any infectious disease that is transmitted (by a vector) from an animal reservoir to a human being.
Infectious agents that cause illness or disease in other living organisms are known as pathogens. These agents may include a wide variety of microorganisms (e.g. mycoplasmas, bacteria, protozoa, spirochetes, and rickettsias) as well as fungi, helminths (roundworms and flatworms), and viruses. A host is any living organism that is infected by a pathogen, regardless of whether or not symptoms of the disease are present. Some hosts die quickly, others may kill or inactivate the pathogen, and still others may retain the pathogen in a condition of readiness to infect other hosts. Whenever a host serves as a source of new infections for other hosts (of the same or different species) it is known as a reservoir. Since pathogens do not have legs or wings, they are often “carried” from one host to another by vectors. Insects and related arthropods are among the most important vectors of pathogens. The term zoonosis (or zoonotic disease) refers to any infectious disease that is transmitted (by a vector) from an animal reservoir to a human being.
Although epidemics of arthropod-borne disease have been well-documented throughout human history, it was not until the late 1800’s that insects and related arthropods were convincingly linked to the spread of human disease. In 1878, Patrick Manson first demonstrated that mosquitoes can transmit filariasis, a disease of the blood and lymph caused by roundworms (nematodes). His research was followed in rapid succession by evidence that Anopheles spp. mosquitoes carry malaria (Ronald Ross, 1897), fleas spread bubonic plague (P. L. Simond, 1898), and mosquitoes, particularly Aedes aegypti, transmit yellow fever (the U. S. Army Yellow Fever Commission headed by Walter Reed, James Carroll, Jesse Lazear, and A. J. Agramonte, 1900). More about
Insect Vectors
of Human Disease Today, we know of over 200 human diseases that can be spread by insects and related arthropods.
Despite the efforts of modern medicine, spread of arthropod-borne disease is still one of the most serious concerns facing public health officials and the medical community in general. The World Health Organization (WHO) estimates that as many as 4 million people die each year from the consequences of arthropod-borne disease. Obviously, the problem is most severe in underdeveloped countries where access to good medical care is limited. But even here in the United States, encephalitis (mosquito-borne), Lyme disease (tick-borne), and Rocky Mountain Spotted Fever (tick-borne) are still regarded as epidemic-scale problems. The Communicable Disease Control Center (CDC) in Atlanta, Georgia estimates that eight out of every ten Americans will be infected by an arthropod-borne disease sometime during their lives. Pathogens coexist in elaborate ecological relationships with their hosts and vectors. Without a vector, the pathogen could not infect new hosts, and without new hosts, the pathogen would eventually become extinct. The term biocenosis (pl. biocenoses) can be used to denote an ecological group that includes a pathogen and all of its hosts and vectors.
Some pathogens may have multiple hosts, reservoirs, or vectors. For example, Pasturella tularensis, the tularemia pathogen, can be transmitted to humans by deer flies, ticks, fleas, or body lice from reservoirs in rodents as well as other humans. Other pathogens, like the Plasmodium species that cause malaria, have a much narrower biocenosis — they survive only as long as they remain within their human hosts and mosquito vectors. Finally, there are pathogens (e.g. the causal agents of cholera and amoebic dysentery) that can survive for long periods outside the bodies of living hosts. These infectious agents are often spread to humans by flies or other insects that visit sewage and garbage.
In some cases, pathogens may simply adhere to a vector’s feet or mouthparts, catching a quick ride to a new host. This is known as mechanical transmission. Most of the pathogens that are transmitted mechanically are able to survive short-term exposure to the atmosphere and sunlight. Many types of arboviruses (short for arthropod-borne viruses) are spread by mechanical transmission on the mouthparts of mosquitoes.
 In contrast, biological transmission occurs when the pathogen survives for a time inside the vector’s body, and is later spread to another host. Some of these pathogens relocate within the body of the vector, traveling from the gut to the salivary glands, for example. Others, such as the rickettsia of rocky mountain spotted fever, remain dormant in the vector’s body and only become activated after feeding commences. Removing a tick within 1-2 hours of attachment usually will ensure too little time for activation and transmission of its pathogens.
In contrast, biological transmission occurs when the pathogen survives for a time inside the vector’s body, and is later spread to another host. Some of these pathogens relocate within the body of the vector, traveling from the gut to the salivary glands, for example. Others, such as the rickettsia of rocky mountain spotted fever, remain dormant in the vector’s body and only become activated after feeding commences. Removing a tick within 1-2 hours of attachment usually will ensure too little time for activation and transmission of its pathogens.
Some pathogens can reproduce in the vector, and a few (the plasmodium of malaria, for example) must complete a part of their life cycle inside the vector’s body. More about
Malaria Newly hatched insects are usually pathogen-free. After feeding on an infected host, the vector may be able to infect new hosts immediately (in the case of mechanical transmission) or there may be a waiting period (latency) of days to weeks (in the case of biological transmission) while the pathogen migrates or reproduces inside the vector’s body. Once infected, a vector may retain the pathogen for the rest of its life (persistent infection) or may eventually eliminate or inactivate the pathogen (non-persistent infection).
Although vectors typically acquire a pathogen only by feeding on an infected host, there are a few species that pass infection through the egg stage from generation to generation. Such transovarial transmission occurs most commonly in ticks.

Edgar Allan Poe
Arthropod-borne diseases have shaped the course of human history. Ever since medieval times, epidemics of bubonic plague have swept through the civilized world. It is estimated that nearly one-fourth of the population of Europe (20-25 million people) died of plague (The Black Death) during the 14th century. Edgar Allan Poe described the gruesome death of plague victims in his story The Masque of the Red Death:
“No pestilence had ever been so fatal or so hideous. Blood was its Avatar and its seal — the redness and the horror of blood. There were sharp pains, and sudden dizziness, and then profuse bleeding at the pores, with dissolution. The scarlet stains upon the body and especially upon the face of the victim, were the pest ban which shut him out from the aid and from the sympathy of his fellow-men.”
Malaria and typhus, both arthropod-borne pathogens, played major roles in the outcome of several wars. In 1815, during Napoleon’s final campaign, his army suffered 105,000 war casualties but lost 219,000 fighting men to typhus. After their rout at Waterloo, one disappointed Frenchman complained that they had been defeated by “General Famine, General Winter, and General Typhus”. Forty years later, in 1856, the Russian army, weakened by tularemia after marching through fly-infested swamps in Turkey, was soundly defeated by the allied forces of Europe to end the Crimean War. More about
Insects and War 1.2 million cases of malaria were treated during the American Civil War (1861-1865) and 8,000 soldiers died. More than 100,000 troops were sidelined with malaria during World War II, yet the Allied army was in much better health than the Japanese largely due to widespread use of a “new” insecticide (DDT) to control lice and mosquitoes. Many historians believe that, even without the atomic bomb, Japan’s army would not have survived much longer against the onslaught of typhus and malaria.

Vladimir Lenin
Demographics and civilization have also been shaped by arthropod-borne disease. Deteriorating socio-economic conditions during the Russian Revolution (1917) prompted Lenin to declare, “Either socialism will defeat the louse, or the louse will defeat socialism.” Even today much of equatorial Africa is uninhabitable because of endemic sleeping sickness vectored by the tsetse fly. The World Health Organization estimates that more than 500 million people throughout the world currently suffer from the debilitating effects of arthropod-borne disease.
 It is impossible to measure the full impact of insects and other arthropods on human health and welfare. These organisms have the capacity to inflict injury, disease, discomfort, or distress. They can be a direct cause of illness, pain, and suffering through bites and stings, infested wounds, or allergic reactions. They feed on blood or body tissues and they may transmit deadly pathogens or parasites. Economic losses associated with these pests are borne not only by the affected individuals and their families, but also by human society in general. Losses include not only the direct costs of medicine and health care, but also indirect costs resulting from stress, absenteeism, and reduced productivity. These are costs that are not easy to measure in dollars and cents.
It is impossible to measure the full impact of insects and other arthropods on human health and welfare. These organisms have the capacity to inflict injury, disease, discomfort, or distress. They can be a direct cause of illness, pain, and suffering through bites and stings, infested wounds, or allergic reactions. They feed on blood or body tissues and they may transmit deadly pathogens or parasites. Economic losses associated with these pests are borne not only by the affected individuals and their families, but also by human society in general. Losses include not only the direct costs of medicine and health care, but also indirect costs resulting from stress, absenteeism, and reduced productivity. These are costs that are not easy to measure in dollars and cents.
 Most mandibulate insects are not strong enough to pierce human skin with their mouthparts. Their bite is usually little more than a pinch, serving primarily as a defensive behavior (e.g. ground beetles and ants). Even fire ants (Solenopsis spp.), whose painful “bite” is well known, lack the ability to penetrate skin. In fact, their “bite” is actually caused by a sting at the other end of the body!
Most mandibulate insects are not strong enough to pierce human skin with their mouthparts. Their bite is usually little more than a pinch, serving primarily as a defensive behavior (e.g. ground beetles and ants). Even fire ants (Solenopsis spp.), whose painful “bite” is well known, lack the ability to penetrate skin. In fact, their “bite” is actually caused by a sting at the other end of the body! Most of these arthropods are hematophagous (they feed on blood). Their mouthparts are designed either to cut the skin and induce bleeding (horse flies and stable flies) or to pierce far enough under the skin to reach capillary blood (mosquitoes, bugs, fleas, etc.). Salivary enzymes and other compounds, such as anti-coagulants, anesthetics, and vasodilators also may be injected by the mouthparts during feeding. The localized reaction to an insect bite (pain, swelling, redness, etc.) is usually a physiological (inflammatory) response to these injected compounds.
Most of these arthropods are hematophagous (they feed on blood). Their mouthparts are designed either to cut the skin and induce bleeding (horse flies and stable flies) or to pierce far enough under the skin to reach capillary blood (mosquitoes, bugs, fleas, etc.). Salivary enzymes and other compounds, such as anti-coagulants, anesthetics, and vasodilators also may be injected by the mouthparts during feeding. The localized reaction to an insect bite (pain, swelling, redness, etc.) is usually a physiological (inflammatory) response to these injected compounds. Although the amount of blood taken by each insect may be quite small, the cumulative effects of blood feeding by large populations of hematophagous insects can be life-threatening. In the summertime, small herds of reindeer living above the arctic circle have died from desanguination (massive loss of blood) caused by hoards of mosquitoes and black flies.
Although the amount of blood taken by each insect may be quite small, the cumulative effects of blood feeding by large populations of hematophagous insects can be life-threatening. In the summertime, small herds of reindeer living above the arctic circle have died from desanguination (massive loss of blood) caused by hoards of mosquitoes and black flies. Some arachnids (e.g. spiders) and most water bugs (Notonectidae, Belostomatidae, and Gerridae, for example) bite only defensively. Their strong, piercing mouthparts can inject toxins or digestive enzymes that may cause pain and localized swelling. In North America, the black widow spider (Latrodectus mactans), the brown recluse spider (Loxosceles reclusa), and two species of scorpions (Centruroides sculpturatus and C. gertschi) are the only arthropods with a venom that is toxic enough to cause serious illness or death.
Some arachnids (e.g. spiders) and most water bugs (Notonectidae, Belostomatidae, and Gerridae, for example) bite only defensively. Their strong, piercing mouthparts can inject toxins or digestive enzymes that may cause pain and localized swelling. In North America, the black widow spider (Latrodectus mactans), the brown recluse spider (Loxosceles reclusa), and two species of scorpions (Centruroides sculpturatus and C. gertschi) are the only arthropods with a venom that is toxic enough to cause serious illness or death. Ants, wasps, bees, and scorpions are the only arthropods that have a true stinger. Some predatory and parasitic insects sting to kill or immobilize their prey, whereas most other species sting only as a defensive behavior to kill or drive away potential predators. In all of the stinging (aculeate) hymenoptera, the stinger is modified from structures of the ovipositor. The shaft of the stinger is hollow, occasionally barbed, and connected internally to a venom gland that produces a complex mixture of compounds that may destroy cells (hemolytic and proteolytic enzymes), increase blood flow (hemorrhagic enzymes), break down intercellular connective tissue (hyaluronidase), and cause neurotoxic or other pharmacologic effects on nerve cells.
Ants, wasps, bees, and scorpions are the only arthropods that have a true stinger. Some predatory and parasitic insects sting to kill or immobilize their prey, whereas most other species sting only as a defensive behavior to kill or drive away potential predators. In all of the stinging (aculeate) hymenoptera, the stinger is modified from structures of the ovipositor. The shaft of the stinger is hollow, occasionally barbed, and connected internally to a venom gland that produces a complex mixture of compounds that may destroy cells (hemolytic and proteolytic enzymes), increase blood flow (hemorrhagic enzymes), break down intercellular connective tissue (hyaluronidase), and cause neurotoxic or other pharmacologic effects on nerve cells. Arthropod venom is rapid-acting and frequently associated with considerable pain. Most people experience an intense local reaction that subsides after several hours and heals within a few days. But for other people (estimates range from 2-5% of the U.S. population) a single sting may elicit anaphylactic shock, a life-threatening allergic reaction caused by hypersensitivity to insect protein or any other venom component. Anaphylaxis is characterized by rapid loss of blood pressure, fainting, and respiratory difficulty. If the patient does not receive prompt medical attention, unconsciousness and death may occur within minutes. Emergency treatment of anaphylactic shock usually consists of deep subcutaneous or intramuscular injections of a cardiac stimulant (such as norepinephrine) in an effort to counteract the physiological reaction, increase heart rate, and stabilize blood pressure. Emergency bee sting kits, containing auto-injectable norepinephrine, are available by prescription to patients with known sensitivity to insect stings. In the United States, about 20 deaths per year are attributed to stinging insects — in nearly every case death results from anaphylactic shock, not the sting itself.
Arthropod venom is rapid-acting and frequently associated with considerable pain. Most people experience an intense local reaction that subsides after several hours and heals within a few days. But for other people (estimates range from 2-5% of the U.S. population) a single sting may elicit anaphylactic shock, a life-threatening allergic reaction caused by hypersensitivity to insect protein or any other venom component. Anaphylaxis is characterized by rapid loss of blood pressure, fainting, and respiratory difficulty. If the patient does not receive prompt medical attention, unconsciousness and death may occur within minutes. Emergency treatment of anaphylactic shock usually consists of deep subcutaneous or intramuscular injections of a cardiac stimulant (such as norepinephrine) in an effort to counteract the physiological reaction, increase heart rate, and stabilize blood pressure. Emergency bee sting kits, containing auto-injectable norepinephrine, are available by prescription to patients with known sensitivity to insect stings. In the United States, about 20 deaths per year are attributed to stinging insects — in nearly every case death results from anaphylactic shock, not the sting itself. The larvae of certain flannel moths (Megalopygidae) and slug caterpillars (Limacodidae) do not have a stinger, but they also inflict a sharp, stinging pain upon contact.
The larvae of certain flannel moths (Megalopygidae) and slug caterpillars (Limacodidae) do not have a stinger, but they also inflict a sharp, stinging pain upon contact. Skin and eye irritation, respiratory inflammation, and various types of chronic allergies may also be caused by insects and related arthropods. An allergic reaction can be induced by nearly any component of an insect’s body, but hairs, scales, exuviae, and fecal products are the most common culprits. Allergies to household dust, for example, can often be traced to dander from fleas (Siphonaptera), cockroaches (Blattodea), or house dust mites (Dermatophagoides spp.). Larvae of the browntail moth (Euproctis chrysorrhoea) have hairs that cause an irritating rash on the skin of many people.
Skin and eye irritation, respiratory inflammation, and various types of chronic allergies may also be caused by insects and related arthropods. An allergic reaction can be induced by nearly any component of an insect’s body, but hairs, scales, exuviae, and fecal products are the most common culprits. Allergies to household dust, for example, can often be traced to dander from fleas (Siphonaptera), cockroaches (Blattodea), or house dust mites (Dermatophagoides spp.). Larvae of the browntail moth (Euproctis chrysorrhoea) have hairs that cause an irritating rash on the skin of many people. Of all the arthropods, only the larvae of certain flies (Diptera) are adapted to invade and consume the tissues of a vertebrate host. An infestation by any of these flies is known as myiasis. In North America, this type of parasitism is most common among domestic animals (particularly sheep, cattle, and horses), but it can also be a problem among the poor and elderly of the human population where it is usually associated with neglect and unsanitary conditions.
Of all the arthropods, only the larvae of certain flies (Diptera) are adapted to invade and consume the tissues of a vertebrate host. An infestation by any of these flies is known as myiasis. In North America, this type of parasitism is most common among domestic animals (particularly sheep, cattle, and horses), but it can also be a problem among the poor and elderly of the human population where it is usually associated with neglect and unsanitary conditions. Larvae of flies in the family Gastrophilidae (the horse bot flies) are internal parasites of horses and mules. Most species lay their eggs around the animal’s nose or mouth. After hatching, the larvae burrow or crawl into the horse’s mouth and eventually move down the digestive tract, attaching themselves to the walls of the stomach, duodenum, or rectum. The horse bot fly (Gasterophilus intestinalis) lays its eggs on the legs, flanks, or shoulders of the horse. These eggs hatch immediately when they are licked and ingested by the horse. The presence of bots (fly larvae) in the animal’s digestive system often causes malnutrition, ulceration of the digestive tract, and even complete blockage of the intestine. Mature larvae leave their vertebrate host by passing out as excrement. They pupate in the soil and emerge as adults several weeks later.
Larvae of flies in the family Gastrophilidae (the horse bot flies) are internal parasites of horses and mules. Most species lay their eggs around the animal’s nose or mouth. After hatching, the larvae burrow or crawl into the horse’s mouth and eventually move down the digestive tract, attaching themselves to the walls of the stomach, duodenum, or rectum. The horse bot fly (Gasterophilus intestinalis) lays its eggs on the legs, flanks, or shoulders of the horse. These eggs hatch immediately when they are licked and ingested by the horse. The presence of bots (fly larvae) in the animal’s digestive system often causes malnutrition, ulceration of the digestive tract, and even complete blockage of the intestine. Mature larvae leave their vertebrate host by passing out as excrement. They pupate in the soil and emerge as adults several weeks later. Infectious agents that cause illness or disease in other living organisms are known as pathogens. These agents may include a wide variety of microorganisms (e.g. mycoplasmas, bacteria, protozoa, spirochetes, and rickettsias) as well as fungi, helminths (roundworms and flatworms), and viruses. A host is any living organism that is infected by a pathogen, regardless of whether or not symptoms of the disease are present. Some hosts die quickly, others may kill or inactivate the pathogen, and still others may retain the pathogen in a condition of readiness to infect other hosts. Whenever a host serves as a source of new infections for other hosts (of the same or different species) it is known as a reservoir. Since pathogens do not have legs or wings, they are often “carried” from one host to another by vectors. Insects and related arthropods are among the most important vectors of pathogens. The term zoonosis (or zoonotic disease) refers to any infectious disease that is transmitted (by a vector) from an animal reservoir to a human being.
Infectious agents that cause illness or disease in other living organisms are known as pathogens. These agents may include a wide variety of microorganisms (e.g. mycoplasmas, bacteria, protozoa, spirochetes, and rickettsias) as well as fungi, helminths (roundworms and flatworms), and viruses. A host is any living organism that is infected by a pathogen, regardless of whether or not symptoms of the disease are present. Some hosts die quickly, others may kill or inactivate the pathogen, and still others may retain the pathogen in a condition of readiness to infect other hosts. Whenever a host serves as a source of new infections for other hosts (of the same or different species) it is known as a reservoir. Since pathogens do not have legs or wings, they are often “carried” from one host to another by vectors. Insects and related arthropods are among the most important vectors of pathogens. The term zoonosis (or zoonotic disease) refers to any infectious disease that is transmitted (by a vector) from an animal reservoir to a human being. In contrast, biological transmission occurs when the pathogen survives for a time inside the vector’s body, and is later spread to another host. Some of these pathogens relocate within the body of the vector, traveling from the gut to the salivary glands, for example. Others, such as the rickettsia of rocky mountain spotted fever, remain dormant in the vector’s body and only become activated after feeding commences. Removing a tick within 1-2 hours of attachment usually will ensure too little time for activation and transmission of its pathogens.
In contrast, biological transmission occurs when the pathogen survives for a time inside the vector’s body, and is later spread to another host. Some of these pathogens relocate within the body of the vector, traveling from the gut to the salivary glands, for example. Others, such as the rickettsia of rocky mountain spotted fever, remain dormant in the vector’s body and only become activated after feeding commences. Removing a tick within 1-2 hours of attachment usually will ensure too little time for activation and transmission of its pathogens.

